Endovascular aneurysm repair
| Endovascular aneurysm repair | |
|---|---|
| Intervention | |
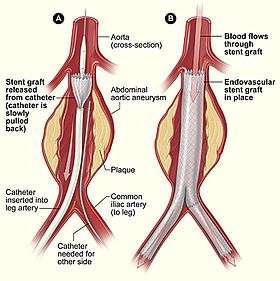 Endovascular aneurysm repair | |
| ICD-9-CM | 39.51, 39.52, 39.7 |
Endovascular aneurysm repair (or endovascular aortic repair) (EVAR) is a type of endovascular surgery used to treat pathology of the aorta, most commonly an abdominal aortic aneurysm (AAA). When used to treat thoracic aortic disease, the procedure is then specifically termed TEVAR (thoracic endovascular aortic/aneurysm repair). The procedure involves the placement of an expandable stent graft within the aorta to treat aortic disease without operating directly on the aorta. In 2003, EVAR surpassed open aortic surgery as the most common technique for repair of AAA,[1] and in 2010, EVAR accounted for 78% of all intact AAA repair in the United States.[2]
Medical uses

Standard EVAR is appropriate for aneurysms that begin below the renal arteries, where there exists an adequate length of normal aorta (the "proximal aortic neck") for reliable attachment of the endograft without leakage of blood around the device ("endoleak").
Patients with aneurysms require elective repair of their aneurysm when it reaches a diameter large enough (typically greater than 5.5 cm) such that the risk of rupture is greater than the risk of surgery. Repair is also warranted for aneurysms that rapidly enlarge or those that have been the source of emboli (debris from the aneurysm that dislodge and travel into other arteries). Lastly, repair is also indicated for aneurysms that are the source of pain and tenderness, which may indicate impending rupture. The options for repair include traditional open aortic surgery or endovascular repair.
Endovascular procedures aim to reduce the morbidity and mortality of treating arterial disease in a patient population that is increasingly older and less fit than when major open repairs were developed and popularized. Even in the early days, significant risks were accepted in the understanding that the large open operation was the only option. That is not the case in most patients today.
Studies that assign aneurysm patients to treatment with EVAR or traditional open surgery have demonstrated fewer early complications with the minimally-invasive approach. Some studies have also observed a lower mortality rate with EVAR.[3][4] The reduction in death, however, does not persist long-term. After a few years the survival after repair is similar with EVAR or open surgery. This observation may be the result of durability problems with early endografts, with a corresponding need for additional procedures to repair endoleaks and other device-related issues. Newer, improved technology may reduce the need for such secondary procedures. If so, the results of EVAR may improve to the point where long-term survival benefit becomes evident.
EVAR is also used for rupture of the abdominal and descending thoracic aorta, and in rare cases used to treat pathology of the ascending aorta.[5]
Aortic dissection
Endografts have been used in patients with aortic dissection, noting the extremely complex nature of open surgical repair in these patients. While the results have been excellent, no significant survival advantage has been demonstrable compared with open surgical repair. In uncomplicated aortic dissections, no benefit has been demonstrated over medical management alone. In uncomplicated type B aortic dissection, TEVAR does not seem either to improve or compromise 2-year survival and adverse event rates.[6] Its use in complicated aortic dissection is under investigation.
Before people are deemed to be a suitable candidate for this treatment, they have to go through a rigorous set of tests. These include a CT scan of the complete thorax/abdomen/pelvis, and blood tests. The CT scan gives precise measurements of the aneurysm and the surrounding anatomy. In particular the calibre/tortuosity of the iliac arteries and the relationship of the neck of the aneurysm to the renal arteries are important determinants of whether the aneurysm is amenable to endoluminal repair. In certain occasions where the renal arteries are too close to the aneurysm, the custom-made fenestrated graft stent is now an accepted alternative to doing open surgery.
Reasons to avoid
A patient's anatomy can be unsuitable for EVAR in several ways. Most commonly, in an infrarenal aneurysm, a potential EVAR candidate lacks adequate length of normal-diameter aorta between the aneurysm and the takeoff of the renal arteries, the "infra-renal neck". Other relative contra-indications include prohibitively small iliac arteries, aneurysmal iliac arteries, prohibitively small femoral arteries, or circumferential calcification of the femoral or iliac arteries.
In addition to a short proximal aortic neck, the neck may be angulated, large in diameter, or shaped like a funnel (conical) where the neck diameter at the top is larger than the neck diameter at the bottom. Along with a short proximal aortic neck, necks with any of these characteristics are called “hostile necks” and endovascular repair can be either contraindicated or associated with early late complications of endoleak, or endograft migration, or both.
Many of the advances in EVAR technique aim to adapt EVAR for these situations, and advanced techniques allow EVAR to be employed in patients who previously were not candidates.
Technique

The procedure is carried out in a sterile environment under x-ray fluoroscopic guidance. It is usually carried out by a vascular surgeon or cardiac surgeon, and occasionally by an interventional radiologist, general surgeon or interventional cardiologist. [7] The procedure can be performed under general, regional (spinal or epidural) or even local anesthesia.
Access to the patient's femoral arteries can be with surgical incisions or percutaneously in the groin on both sides. Vascular sheaths are introduced into the patient's femoral arteries, through which guidewires, catheters and the endograft are passed.
Diagnostic angiography images are captured of the aorta to determine the location of the patient's renal arteries, so the stent graft can be deployed without blocking these. Failure to achieve this will cause renal failure. With most devices, the "main body" of the endograft is placed first, followed by the "limbs" which join the main body and extend to the iliac arteries, effectively protecting the aneurysm sac from blood pressure.
The abdominal aneurysm extends down to the common iliac arteries in about 25%-30% of patients. In such cases, the iliac limbs can be extended into the external iliac artery to bypass a common iliac aneurysm. Alternatively, a specially designed endograft, (an iliac branch device) can be used to preserve flow to the internal iliac arteries. The preservation of the hypogastric (internal iliac) arteries is important to prevent buttock claudication and impotence, and every effort should be made to preserve flow to at least one hypogastric artery.
The endograft acts as an artificial lumen for blood to flow through, protecting the surrounding aneurysm sac. This reduces the pressure in the aneurysm, which itself will usually thrombose and shrink in size over time.[8]
Staging such procedures is common, particularly to address aortic branch points near the diseased aortic segment. One example in the treatment of thoracic aortic disease is revascularization of the left common carotid artery and/or the left subclavian artery from the innominate artery or the right common carotid artery to allow treatment of a thoracic aortic aneurysm that encroaches proximally into the aortic arch. These "extra-anatomic bypasses" can be performed without an invasive thoracotomy. Another example in the abdominal aorta is the embolization of the internal iliac artery on one side prior to coverage by an iliac limb device. Continued design improvement in stent graft including branched endografts will reduce but not eliminate multi-stage procedures.
Percutaneous EVAR
Standard EVAR involves a surgical cut-down on either the femoral or iliac arteries, with the creation of a 4–6 cm incision. Like many surgical procedures, EVAR has advanced to a more minimally invasive technique, by accessing the femoral arteries "percutaneously". In percutaneous EVAR (PEVAR), small, sub-centimeter incisions are made over the femoral artery, and endovascular techniques are used to place the device over a wire. Evidence favoring this technique is lacking, but studies are ongoing.[9]
Fenestrated EVAR
In certain occasions, a specially designed custom-made graft device ("endograft"), which has holes (fenestrations) on the graft body to maintain the patency of the visceral arteries, is used for the procedure, which is called FEVAR (fenestrated endovascular aortic/aneurysm repair). When the aneurysm begins at close to the renal arteries, standard EVAR may be contraindicated since there will be an inadequate length of suitable aorta for the endograft attachment. In these cases a fenestrated endograft may be useful, where the attachment of the endograft to the aorta may be placed above the renal arteries with each fenestration opposite a renal artery so that blood flow to the kidneys is maintained. Fenestrated EVAR has been in use in the United Kingdom for over a decade and nationwide early results have been published in the journal Circulation in Jun 2012. [10]
Branched EVAR
Thoraco-abdominal aortic aneurysms (TAAA) involve the aorta in the chest and abdomen. As such, major branch arteries to the head, arms, spinal cord, intestines and kidneys may originate from the aneurysm. An endovascular repair of a TAAA is only possible if blood flow to these critical arteries is preserved. Hybrid procedures offer one option, but a more direct approach involves the use of a branched endograft. Dr. Timothy Chuter pioneered this approach, with a completely endovascular solution. After partial deployment of the main body of an endograft, separate endograft limbs are deployed from the main body to each major aortic branch. This procedure is long, technically difficult, and currently only performed in a few centers. When the aneurysm begins above the renal arteries, neither fenestrated endografts nor EndoAnchoring of an infrarenal endograft are useful (an open surgical repair may be necessary). Alternatively, a "branched" endograft may be used. A branched endograft has graft limbs that branch off of the main portion of the device to directly provide blood flow to the kidneys or the visceral arteries.
Hybrid Procedures
On occasion there is inadequate length or quality of the proximal or distal aortic neck. In these cases, a fully minimally invasive option is not possible. One solution, however, is a hybrid repair, which combines an open surgical bypass with EVAR or TEVAR. In hybrid procedures, the endograft is positioned over major aortic branches. While such a position would normally cause problems from disruption of blood flow to the covered branches (renal, visceral, or branches to the head or arms), the prior placement of bypass grafts to these critical vessels allowed deployment of the endograft at a level that would otherwise not be possible.
If a patient has calcified or narrow femoral arteries that prohibit the introduction of the endograft transfemorally, an iliac conduit may be used. This is typically a piece of PTFE that is sewn directly to the iliac arteries, which are exposed via an open retroperitoneal approach. The endograft is then introduced into the aorta through the conduit.
In patients with thoracic aortic disease involving the arch and descending aorta, it is not always possible to perform a completely endovascular repair. This is because head vessels of the aortic arch supplying blood to the brain cannot be covered and for this reason there in often an inadequate landing zone for stent graft delivery. A hybrid repair strategey offers a reasonable choice for treating such patients. A commonly used hybrid repair procedure is the frozen elephant trunk repair.[11] This technique involves midline sternotomy. The aortic arch is transected and the stent graft device is delivered in an ante-grade fashion in the descending aorta. The aortic arch is subsequently reconstructed and the proximal portion of the stent graft device is then directly sutured into the surgical graft. Patients with anomalies of the arch and some disease extension into the descending of aorta are often ideal candidates. Studies have reported successful use of hybrid techniques for treating Kommerell Diverticulum[12] and descending aneurysms in patients with previous coarctation repairs.[13][14]
In addition, hybrid techniques combining both open and endovascular repair are also used in managing emergency complications in the aortic arch such as retrograde ascending dissection and endoleaks from previous stent grafting of descending aorta. A reversese frozen elephant trunk repair is shown to be particularly effective.[15]
Adjunctive Procedures in EVAR
- Snorkel: A covered stent placed into a visceral vessel adjacent to the main body of the EVAR device. The aortic lumen of the visceral stent is directed superiorly, resembling a snorkel.
- Chimney: In TEVAR, a covered stent placed from the ascending aorta to a great vessel (e.g., innominate artery) and adjacent to the main body of the EVAR is termed a chimney. In anatomic position, blood flows superiorly through a chimney-stent-graft into the great vessel, just as smoke flows up a chimney.
- Periscope: Like a snorkel, a periscope stent-graft provides flow to a visceral vessel, but in retrograde fashion, with the aortic lumen inferior to the main body of the EVAR device.
- Stents: Large bare-metal stents has been used to treat proximal endoleaks, as have aortic extension cuffs to treat endograft migration.
- Glue: Trans-catheter embolic glue has been used to treat type I endoleaks, with inconsistent success.[16]
- EndoAnchors: Small, helically-shaped devices are screwed through the endograft and into the aortic wall. EndoAnchors have been used successfully to treat endoleaks and, in concert with an aortic extension endograft, to treat migration of the original endograft.[17] Rigorous evaluations and long-term outcomes of this technique are not yet available.
Risks
The complications of EVAR can be divided into those that are related to the repair procedure and those related to the endograft device. For example, a myocardial infarction that occurs immediately after the repair is normally related to the procedure and not the device. By contrast, the development of an endoleak from degeneration of endograft fabric would be a device-related complication.
Durability and problems such as 'endoleaks' may require careful surveillance and adjuvant procedures to ensure success of the EVAR or EVAR/hybrid procedure. CT Angiography (CTA) imaging has in particular made a key contribution to planning, success, durability in this complex area of vascular surgery.
A major cause of complications in EVAR is the failure of the seal between the proximal, infra-renal aneurysm neck and the endovascular graft.[18][19][20] Risk of this form of failure is especially elevated in adverse or challenging proximal neck anatomies, where this seal could be compromised by unsuitable geometric fit between the graft and vessel wall, as well as instability of the anatomy.[21][22][23] New recent techniques have been introduced to address these risks by utilizing a segment of the supra-renal portion of the aorta to increase the sealing zone, such as with fenestrated EVAR, chimneys and snorkels.[24] These techniques may be suitable in certain patients with qualifying factors, e.g., configuration of renal arteries, renal function. However, these are more complex procedures than standard EVAR and may be subject to further complications.[25][26][27]
An approach that directly augments the fixation and sealing between the graft and aorta to mimic the stability of a surgical anastomosis is EndoAnchoring.[28][29] EndoAnchors are small, helically shaped implants that directly lock the graft to the aortic wall with the goal to prevent complications of the seal, especially in adverse neck anatomies.[30][31] These EndoAnchors may also be used to treat identified leaks between the graft and proximal neck.[32][33][34]
Procedure related
Arterial dissection,contrast-induced renal failure, thromboembolizaton, ischemic colitis, groin hematoma, wound infection, type II endoleaks, myocardial infarction, congestive heart failure, cardiac arrhythmias, respiratory failure.
Device related
Endograft migration, aneurysm rupture, graft limb stenosis/kinking, type I/III/IV endoleaks
Endoleaks
An endoleak is a leak into the aneurysm sac after endovascular repair. Five types of endoleaks exist:[8]
- Type I - Perigraft leakage at proximal or distal graft attachment sites (near the renal and iliac arteries)
- Type II - Retrograde flow to the aneurysm sac from branches such as the lumbar and inferior mesenteric arteries. Type II endoleaks are the most common, and least serious type of endoleak. Type II endoleaks do not require immediate treatment, as a portion will resolve spontaneously.
- Type III - Leakage between overlapping parts of the stent (i.e., connection between overlapping components) or rupture through graft material.
- Type IV - Leakage through the graft wall due to the quality (porosity) of the graft material. Seen in first-generation grafts, changes in graft material in modern devices have decreased the prevalence of type IV leaks.
- Type V - Expansion of the aneurysm sac without an identifiable leak. Also called "endotension".
Recovery after EVAR
Unlike traditional aortic repair, standard recovery after EVAR is remarkably straightforward. Patients who have undergone EVAR typically spend one night in the hospital to be monitored, although it has been suggested that EVAR can be performed as a same-day procedure.[35]
Patients are advised to slowly return to normal activity. There are no specific activity restrictions after EVAR, however patients typically are seen by their surgeon within one month after EVAR to begin post-EVAR surveillance.
History
Noting the morbidity of open surgical repair of aortic aneurysms, particularly in the elderly and medically fragile patient, Dr. Nicholas Volodos working in Kharkov, Soviet Union developed the first aortic endograft. His work started in 1970s–'80s with experimental development of fabric covered Z-stent, which was first bench-tested and then implanted in dogs. Both devices: Z-stents and fabric-covered stents were patented (in the Soviet Union) on May 22, 1984. They were the result of a rather rigorous and extensive pre-clinical multi-year process that included in-depth analysis of physical and physiologic characteristics of various stent designs, testing in a flow model, and animal implantations (with 6-month follow-up and detailed studies on explanted devices). First human implant of the fabric-covered Z-stent in 1985 for treatment of iliac artery stenosis. First aortic implantation on March 24, 1987 for treatment of a post-traumatic thoracic aortic aneurysm. Later in 1987, they performed the world’s first EVAR procedure for treatment of AAA (in Kharkov). In 1991, Volodos performed a hybrid transthoracic operation with antegrade delivery and deployment (through the ascending aorta) of a stent-graft to treat a post-coarctation pseudoaneurysm of the proximal descending thoracic aorta.By the early 1990s, Volodos and his associates had accumulated a rather large clinical experience (of 100 cases or more) with stent-graft implantations in the abdominal and thoracic aorta and in other arterial beds. Volodos presented his research at international meeting and published in 1988.[36]
Parodi introduced the endovascular aneurysm repair to the western world and performed the first successful endovascular repair of an abdominal aortic aneurysm in 1990.
The modern endovascular device used to repair abdominal aortic aneurysms, which is bifurcated and modular, was pioneered and first employed by Dr. Timothy Chuter while a fellow at the University of Rochester.[37] The first clinical series of his device was published from Nottingham in 1994.[38] The first endovascular repair of a ruptured abdominal aortic aneurysm was also reported from Nottingham in 1994.[39]
By 2003, 4 devices were on the market in the United states. [40] Each of these devices has since been either abandoned or further refined to improve its characteristics in vivo.
Special Populations
Women
Women are known to have smaller aortas on average than men, so are potential candidates for AAA treatment at smaller maximum aneurysm diameters than men.
Transplant candidates
As immunosuppressive medications are known to increase the rate of aneurysm growth, transplant candidates are AAA repair candidates at smaller maximum aneurysm diameters than the general population.
Other Animals
Due to the expense associated with EVAR stent graft devices and their specificity to human aortic anatomy, EVAR is not used in other animals.
References
- ↑ Sethi RK, Henry AJ, Hevelone ND, Lipsitz SR, Belkin M, Nguyen LL (September 2013). "Impact of hospital market competition on endovascular aneurysm repair adoption and outcomes.". J. Vasc. Surg. 58 (3): 596–606. doi:10.1016/j.jvs.2013.02.014. PMID 23684424.
- ↑ Dua, A (2014). "Epidemiology of aortic aneurysm repair in the United States from 2000 to 2010". J Vasc Surg. 59 (6): 1512–7. doi:10.1016/j.jvs.2014.01.007. PMID 24560865.
- ↑ Jackson, Rubie (Apr 2012). "Comparison of Long-term Survival After Open vs Endovascular Repair of Intact Abdominal Aortic Aneurysm Among Medicare Beneficiaries". JAMA. 307 (15): 1621–8. doi:10.1001/jama.2012.453. PMID 22511690.
- ↑ Schermerhorn, Marc (January 2008). "Endovascular vs. open repair of abdominal aortic aneurysms in the Medicare population.". New England Journal of Medicine. 358 (5): 464–74. doi:10.1056/NEJMoa0707348. PMID 18234751.
- ↑ McCallum, JC; Limmer, KK; Perricone, A; Bandyk, D; Kansal, N (July 2013). "Total endovascular repair of acute ascending aortic rupture: a case report and review of the literature.". Vascular and Endovascular Surgery. 47 (5): 374–8. doi:10.1177/1538574413486838. PMID 23697343.
- ↑ Nienaber CA, Rousseau H, Eggebrecht H, et al. (December 2009). "Randomized comparison of strategies for type B aortic dissection: the INvestigation of STEnt Grafts in Aortic Dissection (INSTEAD) trial". Circulation. 120 (25): 2519–28. doi:10.1161/CIRCULATIONAHA.109.886408. PMID 19996018.
- ↑ McCutcheon BA, Talamini MA, Chang DC, Rose JA, Bandyk DF, Wilson SE (September 2013). "The comparative effectiveness of surgeons over interventionalists in endovascular repairs of abdominal aortic aneurysm.". Ann. Surg. 258 (3): 476–82. doi:10.1097/SLA.0b013e3182a196b5. PMID 24022440.
- 1 2 Greenhalgh RM, Powell JT (2008). "Endovascular repair of abdominal aortic aneurysm". N. Engl. J. Med. 358 (5): 494–501. doi:10.1056/NEJMct0707524. PMID 18234753.
- ↑ Jackson, A; Yeoh, SE; Clarke, M (27 February 2014). "Totally percutaneous versus standard femoral artery access for elective bifurcated abdominal endovascular aneurysm repair.". The Cochrane database of systematic reviews. 2: CD010185. doi:10.1002/14651858.CD010185.pub2. PMID 24578199.
- ↑ British Society for Endovascular Therapy and the Global Collaborators on Advanced Stent-Graft Techniques for Aneurysm Repair (GLOBALSTAR) Registry. Early results of fenestrated endovascular repair of juxtarenal aortic aneurysms in the United Kingdom. Circulation. 2012 Jun 5;125(22):2707-15. doi: 10.1161/CIRCULATIONAHA.111.070334. Correspondence to S R Vallabhaneni.
- ↑ Lima, B., Roselli, E. E., Soltesz, E. G., Johnston, D. R., Pujara, A. C., Idrees, J., & Svensson, L. G. (2012). Modified and “reverse” frozen elephant trunk repairs for extensive disease and complications after stent grafting. The Annals of thoracic surgery, 93(1), 103-109.
- ↑ Idrees, J., Keshavamurthy, S., Subramanian, S., Clair, D. G., Svensson, L. G., & Roselli, E. E. (2014). Hybrid repair of Kommerell diverticulum. The Journal of thoracic and cardiovascular surgery, 147(3), 973-976.
- ↑ Idrees, J., Arafat, A., Svensson, L. G., Clair, D., & Roselli, E. E. (2014). Hybrid repair of aortic aneurysm in patients with previous coarctation. The Journal of thoracic and cardiovascular surgery, 148(1), 60-64.
- ↑ Roselli, E. E., Qureshi, A., Idrees, J., Lima, B., Greenberg, R. K., Svensson, L. G., & Pettersson, G. (2012). Open, hybrid, and endovascular treatment for aortic coarctation and postrepair aneurysm in adolescents and adults. The Annals of thoracic surgery, 94(3), 751-758.
- ↑ Idrees, J., Arafat, A., Johnston, D. R., Svensson, L. G., & Roselli, E. E. (2014). Repair of retrograde ascending dissection after descending stent grafting. The Journal of thoracic and cardiovascular surgery, 147(1), 151-154.
- ↑ Eberhardt KM, Sadeghi-Azandaryani M, Worlicek S, Koeppel T, Reiser MF, Treitl M (2014). "Treatment of type I endoleaks using transcatheter embolization with onyx". J Endovasc Ther. 21 (1): 162–71.
- ↑ Deaton DH (2012). "Improving proximal fixation and seal with the HeliFx Aortic EndoAnchor". Semin Vasc Surg. 25 (4): 187–92. doi:10.1053/j.semvascsurg.2012.09.002.
- ↑ Greenhalgh RM, Brown LC, Powell JT, Thompson SG, Epstein D, Sculpher MJ (May 2010). "Endovascular versus open repair of abdominal aortic aneurysm. United Kingdom EVAR Trial Investigators". N Engl J Med. 362 (20): 1863–71. doi:10.1056/nejmoa0909305.
- ↑ De Bruin JL, et al. (2010). "Long-term outcome of open or endovascular repair of abdominal aortic aneurysm". N Engl J Med. 362: 1881–9. doi:10.1056/nejmoa0909499.
- ↑ Becquemin JP, et al. (May 2011). "A randomized controlled trial of endovascular aneurysm repair versus open surgery for abdominal aortic aneurysms in low- to moderate-risk patients". J Vasc Surg. 53 (5): 1167–1173. doi:10.1016/j.jvs.2010.10.124.
- ↑ Leurs LJ, et al. (2006). "Influence of infrarenal neck length on outcome of endovascular abdominal aortic aneurysm repair". J Endovasc Ther. 13 (5): 640–8. doi:10.1583/06-1882.1.
- ↑ Aburahma AF, et al. (2009). "The correlation of aortic neck length to early and late outcomes in endovascular aneurysm repair patients". J Vasc Surg. 50 (4): 738–48. doi:10.1016/j.jvs.2009.04.061.
- ↑ Sternbergh WC, et al. (2002). "Aortic neck angulation predicts adverse outcome with endovascular abdominal aortic aneurysm repair". J Vasc Surg. 35 (3): 482–6. doi:10.1067/mva.2002.119506.
- ↑ Deaton DH (Jun 2009). "Future technologies to address the failed endoprosthesis". Semin Vasc Surg. 22 (2): 111–8. doi:10.1053/j.semvascsurg.2009.04.010.
- ↑ Comparison of outcomes with open, fenestrated, and chimney graft repair of juxtarenal aneurysms: are we ready for a paradigm shift? Katsargyris A, Oikonomou K, Klonaris C, Töpel I, Verhoeven EL. J Endovasc Ther. 2013 Apr;20(2):159-69. doi: 10.1583/1545-1550-20.2.159. Review
- ↑ Technical aspects, current indications, and results of chimney grafts for juxtarenal aortic aneurysms. Coscas R, Kobeiter H, Desgranges P, Becquemin JP. J Vasc Surg. 2011 Jun;53(6):1520-7.
- ↑ Fenestrated endovascular aneurysm repair. Cross J, Gurusamy K, Gadhvi V, Simring D, Harris P, Ivancev K, Richards T. Br J Surg. 2012 Feb;99(2):152-9
- ↑ Melas; et al. (2012). "Helical Endostaples Enhance Endograft Fixation in an Experimental Model Using Human Cadaveric Aortas". J Vasc Surg. 55 (6): 1726–1733. doi:10.1016/j.jvs.2011.11.048.
- ↑ Deaton DH (Dec 2012). "Improving proximal fixation and seal with the HeliFx Aortic EndoAnchor". Semin Vasc Surg. 25 (4): 187–92. doi:10.1053/j.semvascsurg.2012.09.002.
- ↑ De Vries JP, et al. (Feb 2014). "Rationale of EndoAnchors in abdominal aortic aneurysms with short or angulated necks". J Cardiovasc Surg (Torino). 55 (1): 103–7.
- ↑ Perdikides et al "Primary EndoAnchoring in the Endovascular Repair of Abdominal Aortic Aneurysms With an Unfavorable Neck" J Endovasc Ther 2012; 19.
- ↑ Successful Treatment of a Proximal Type I Endoleak with HeliFX EndoAnchors. Hogendoorn W et al. Ann Vasc Surg 2013.
- ↑ Kasprzak P, et al. (2013). "EndoAnchor Placement in Thoracic and Thoracoabdominal Stent-Grafts to Repair Complications of Nonalignment". J Endovasc Therapy. 20: 471–480. doi:10.1583/12-4125.1.
- ↑ Use of endostaples to secure migrated endografts and proximal cuffs after failed endovascular abdominal aortic aneurysm repair. de Vries et al J Vasc Surg. 2011;54:1792-1794.
- ↑ Lachat ML, Pecoraro F, Mayer D, et al. (November 2013). "Outpatient endovascular aortic aneurysm repair: experience in 100 consecutive patients". Ann. Surg. 258 (5): 754–8; discussion 758–9. doi:10.1097/SLA.0b013e3182a617f1. PMID 24045449.
- ↑ Volodos' NL, Karpovich IP, Shekhanin VE, Troian VI, Iakovenko LF (1988). "[A case of distant transfemoral endoprosthesis of the thoracic artery using a self-fixing synthetic prosthesis in traumatic aneurysm]". Grudn Khir (6): 84–6. PMID 3220297.
- ↑ Chuter TA, Green RM, Ouriel K, Fiore WM, DeWeese JA (August 1993). "Transfemoral endovascular aortic graft placement". J. Vasc. Surg. 18 (2): 185–95; discussion 195–7. PMID 8350427.
- ↑ SW Yusuf, DM Baker, TAM Chuter, SC Whitaker, PW Wenham, BR Hopkinson TRANSFEMORAL ENDOLUMINAL REPAIR OF ABDOMINAL AORTIC ANEURYSM WITH BIFURCATED GRAFT Lancet 1994; 344: 650-651.
- ↑ S W Yusuf, S C Whitaker, TAM Chuter, PW Wenham, BR Hopkinson EMERGENCY ENDOVASCULAR ABDOMINAL AORTIC ANEURYSM REPAIR (letter) Lancet 1994; 344: 1645
- ↑ Rutherford, RB (March 2012). "Open versus endovascular stent graft repair for abdominal aortic aneurysms: an historical view.". Seminars in vascular surgery. 25 (1): 39–48. PMID 22595481.
External links
- Society of Interventional Radiology
- Society for Vascular Surgery (U.S.)
- The EVAR Trial: Data and Information
- Information for patients
- Division of Vascular Surgery and Endovascular Therapy at the Baylor College of Medicine